Understanding the Anatomy Behind a Graftless Implant Solution
Pterygoid implants anatomy refers to the three-dimensional relationship between specialized dental implants and the bony structures they engage in the posterior upper jaw. Here’s what you need to know:
Key Anatomical Components:
- Maxillary Tuberosity – The starting point where the implant enters
- Pyramidal Process of Palatine Bone – The middle section providing cortical bone engagement
- Pterygoid Process of Sphenoid Bone – The final anchor point composed of dense cortical bone
- Greater Palatine Canal (GPC) – Contains vital blood vessels and nerves that must be avoided during placement
Why This Anatomy Matters:
- The pterygoid process offers bone density 139% greater than the maxillary tuberosity
- Implants engage 8-9 mm of dense cortical bone when placed at proper angulation
- This unique pathway allows implant placement without sinus lifts or bone grafts
The posterior upper jaw presents one of implant dentistry’s toughest challenges. When teeth are lost in this area, the maxillary sinus expands and the remaining bone shrinks away—sometimes leaving barely enough structure to place traditional implants. For decades, this meant patients faced lengthy bone grafting procedures or complex sinus lift surgeries before they could receive implants.
Pterygoid implants changed this equation entirely.
These specialized implants take a different path through the jaw, anchoring into the pterygoid region—a zone of exceptionally dense bone that resists the resorption affecting other areas. First described by Dr. Jean-François Tulasne in 1992, this graftless approach bypasses the maxillary sinus completely, engaging three distinct bones to create a stable foundation for tooth replacement.
But success depends entirely on understanding the anatomy. The implant must steer between vital structures, engage the right bone at the correct angle, and avoid injury to nearby nerves and blood vessels. Get it right, and patients can achieve survival rates up to 99% with significantly reduced treatment time. Get it wrong, and serious complications can occur.
I’m Dr. Nina Izhaky, and at Tribeca Dental Studio, we’ve made advanced implant solutions like pterygoid placement a cornerstone of our practice by combining state-of-the-art CBCT imaging with meticulous attention to pterygoid implants anatomy. My team and I use detailed three-dimensional planning to ensure every implant engages the optimal bone pathway while maintaining safe distances from critical structures.

The Core of Pterygoid Implants Anatomy
The pterygomaxillary region, located in the very back of your upper jaw, is a fascinating and complex area that holds the key to successful pterygoid implants anatomy. Unlike other areas of the maxilla, which often suffer from significant bone loss after tooth extraction, this region typically maintains a robust supply of dense cortical bone. This superior bone quality is what makes it an ideal site for implant anchorage, providing the stability needed for long-term success.
The surgical pathway for pterygoid implants is unique. Rather than relying on the softer, more porous bone of the alveolar ridge, these implants are designed to traverse the maxillary tuberosity, pass through the pyramidal process of the palatine bone, and ultimately anchor into the cortical plates of the pterygoid process of the sphenoid bone. This multi-bone engagement creates a strong, tripod-like support that can withstand significant chewing forces. For an in-depth look at the intricate vascular and neural structures in this region, we often refer to detailed studies like this anatomical study of pterygoid implants: artery and nerve. Understanding this complex anatomical interplay is paramount to minimizing risks and maximizing the benefits for our patients. If you’re curious about traditional bone grafting options, you can find more info about Bone Grafting services on our website.
Key Anatomical Structures for Placement
Let’s break down the individual bony players involved in pterygoid implants anatomy:
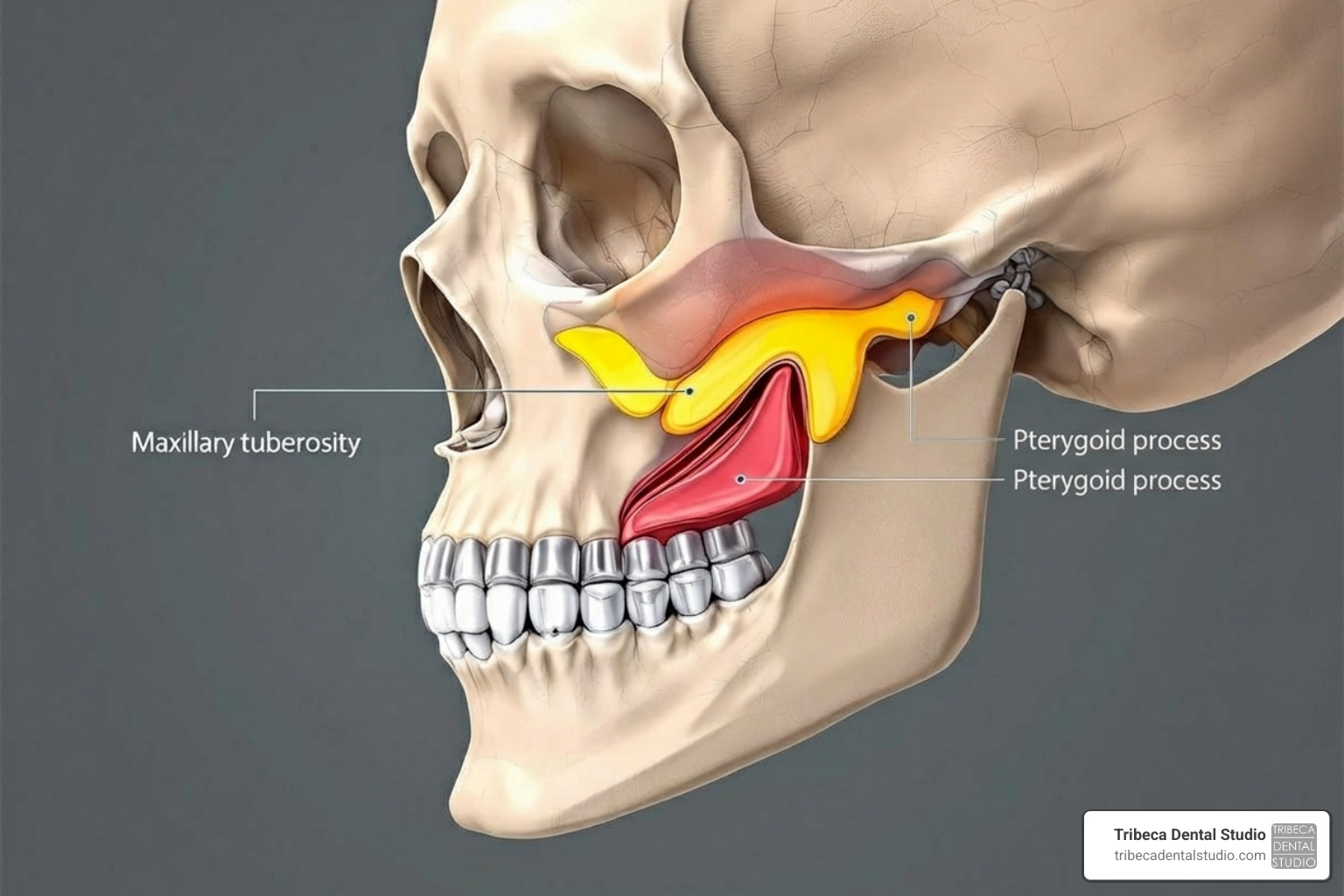
- Maxillary Tuberosity: This is the rounded eminence at the posterior aspect of the maxilla. It’s the initial entry point for the implant. While its bone density can be variable, especially in atrophic maxillae, it serves as the gateway to the denser structures beyond.
- Pyramidal Process of Palatine Bone: Situated behind the maxillary tuberosity, this process of the palatine bone provides a crucial segment of cortical bone for the implant to engage. It acts as an important intermediary anchor.
- Pterygoid Process of Sphenoid Bone: This is the ultimate target for pterygoid implants. Composed of two plates (medial and lateral pterygoid plates) that project downwards from the sphenoid bone, this area offers dense cortical bone, providing excellent primary stability for the implant. The implant typically engages the junction of these plates.
- Pterygoid Fossa: This depression lies between the medial and lateral pterygoid plates. While the implant aims for the dense bone of the process, understanding the surrounding fossa is important for surgical orientation.
The goal is to achieve strong cortical bone engagement within these structures. This ensures that the implant is firmly integrated, a critical factor for immediate loading and long-term stability.
Understanding Bone Density and Morphology
When it comes to dental implants, bone density is everything. It dictates the primary stability of the implant and its long-term success. In the posterior maxilla, the maxillary tuberosity is notorious for having some of the lowest bone density in the oral cavity. This often makes traditional implant placement challenging without extensive preparatory procedures.
However, the pterygoid process is a different story. Research consistently shows that the bone density of the pterygoid process is always greater than that of the maxillary tuberosity. In fact, one study highlighted that the pterygoid area’s bone density was 139.2% higher than in the tuberosity area. This significant difference is precisely why pterygoid implants are so effective: they tap into a high-quality bone reservoir that remains even in severely atrophic cases.
The morphology of the pterygomaxillary region also plays a crucial role. Studies have measured the mean width of the pterygomaxillary joint at 7.51 mm (SD 1.0 mm) and the mean height at 12.5 mm (SD 1.8 mm), with a mean volume of 321.76 mm3 (SD 142.02 mm3). These dimensions provide ample space for implant placement when planned correctly.
Factors like age, sex, and dental status can influence these characteristics. For instance, older patients tend to have less density in the maxillary tuberosity. Interestingly, in dentate patients, the bone density of the middle section of the pterygomaxillary fissure can actually increase with age (Pearson’s correlation = 0.46, P = 0.01). However, in edentulous patients, especially females, bone density in the maxillary tuberosity’s middle section was found to be significantly lower (559.7 GSD) than in males (631.1 GSD). These variations underscore the need for personalized treatment planning, which we prioritize at Tribeca Dental Studio.
Navigating Vital Structures: The Greater Palatine Canal (GPC)
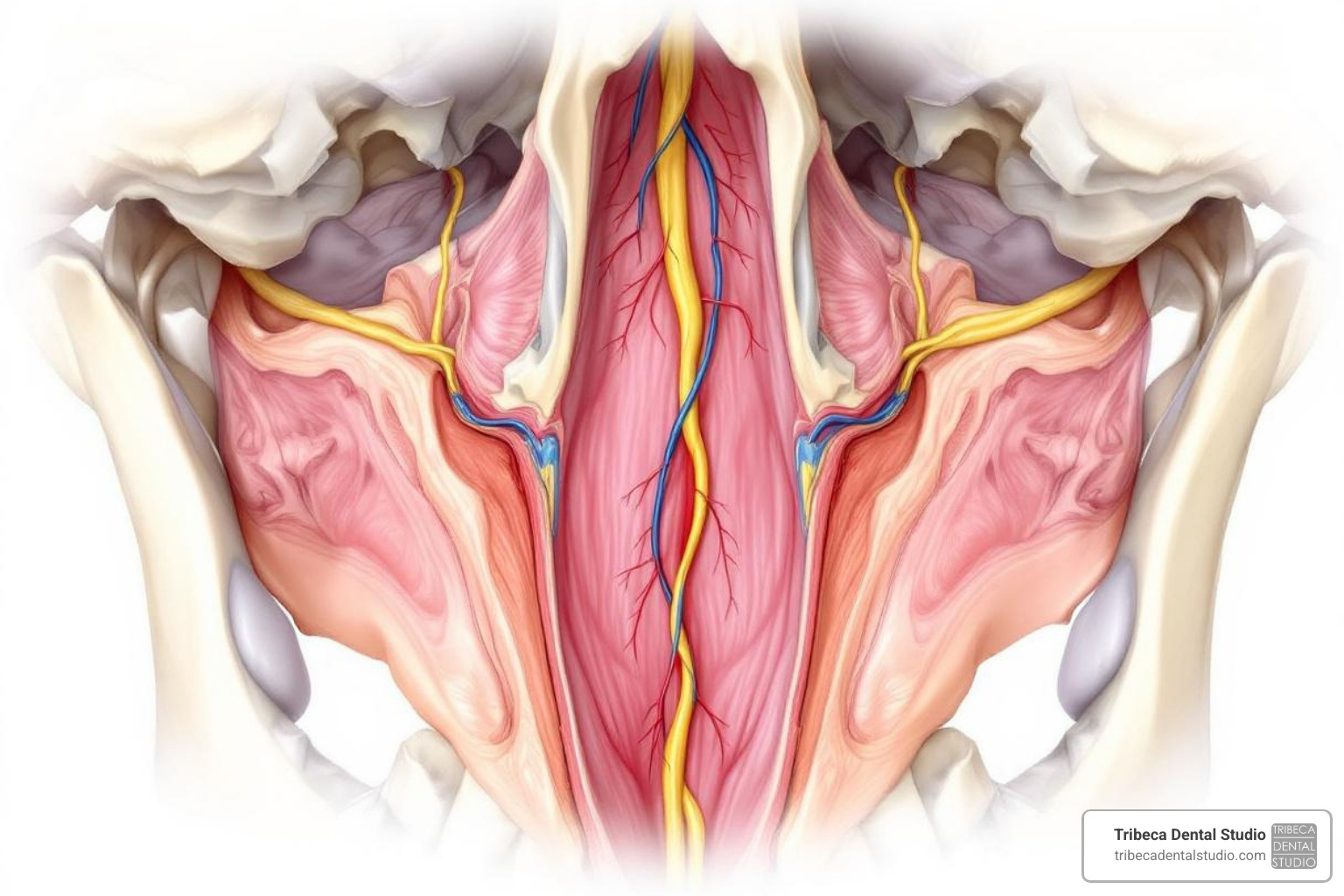
One of the most critical aspects of pterygoid implants anatomy that demands meticulous attention is the Greater Palatine Canal (GPC). This bony tunnel serves as a conduit for the descending palatine artery and the greater palatine nerve, both vital structures that must be protected during implant placement. Injury to these can lead to complications such as bleeding or sensory disturbances.
The GPC’s anatomy presents a unique challenge: its medial wall often communicates with the nasal cavity through bone dehiscence. Studies have found this dehiscence near the inferior nasal concha in a staggering 72.4% of cadavers (21/29). This means there’s a high chance that the canal is not fully enclosed by bone, potentially exposing the artery and nerve directly to the surgical field or allowing communication with the nasal passages.
Within the GPC, the greater palatine nerve consistently passes medial to the descending palatine artery. This anatomical arrangement has a significant clinical implication: if the GPC is inadvertently perforated during surgery, the descending palatine artery is more likely to be damaged first, rather than the greater palatine nerve. While this might sound like a minor detail, it helps surgeons anticipate and manage potential complications. Any perforation could lead to bleeding into the nasal mucosa and potentially spread inflammation to the nasal cavity.
The distance from the Greater Palatine Foramen (GPF), the opening of the GPC, to the posterior end of the maxillary tuberosity averages 11.44 ± 2.56 mm, and to the medial surface of the maxillary tuberosity, it’s 4.28 ± 1.19 mm. These measurements highlight the close proximity of the GPC to the implant placement site, emphasizing the need for precise surgical planning and execution. We always ensure a safety space of at least 2 mm between the implant and these vital neurovascular structures.
Recommended Angulation and Imaging for Pterygoid Implants Anatomy
Precision is paramount in pterygoid implants anatomy. The success of these implants hinges on their exact angulation and trajectory. Historically, a 45° angulation relative to the occlusal plane was often recommended. However, more recent research, including detailed 3D studies, suggests that an angulation closer to the natural bone pillar (pterygoid process and maxillary tuberosity) might be more biomechanically favorable.
Studies indicate that the average inclination of this bone pillar is between 67.3° and 75.1° relative to the Frankfort plane. One study even found a mean implant angulation of 72.5° ± 4.9° in the anteroposterior axis and 64.3° ± 4.99° in the buccopalatal axis relative to the Frankfort plane. An angulation that aligns more closely with the natural bone structure, often around 70-80 degrees relative to the Frankfort plane, can lead to better occlusal force transmission and long-term implant stability. This is a significant shift from older recommendations, as a 45° angulation can decrease implant load capacity by up to 50% compared to a 90° axial placement. The implant’s long axis should typically be inclined slightly toward the palatal side to follow the cortical palatal bone.
To achieve this level of precision, advanced imaging techniques are indispensable. Cone Beam Computed Tomography (CBCT) imaging is highly recommended for planning pterygoid implant surgery. CBCT provides detailed three-dimensional views of the bone structure, maxillary sinus, and vital anatomical landmarks, allowing us to virtually plan the implant placement with millimeter accuracy. This pre-surgical planning is crucial for identifying the optimal implant length (often 15 mm or 18 mm for maximum engagement) and angulation, as well as establishing safety margins to avoid critical structures like the GPC.
At Tribeca Dental Studio, we leverage cutting-edge CBCT technology to perform virtual implant planning, ensuring that each pterygoid implant is placed with the utmost precision and safety. This meticulous approach is part of our commitment to personalized care and successful outcomes. To learn more about our advanced planning, explore our page on Guided Dental Implant Surgery.
Surgical and Prosthetic Advantages of Pterygoid Implants
Pterygoid implants offer a compelling solution for patients with significant bone loss in the posterior maxilla, largely due to their ability to circumvent the need for traditional bone augmentation procedures. This translates into several significant advantages for our patients in Manhattan and Tribeca.
A primary benefit is avoiding sinus elevation. The traditional approach to placing implants in the posterior maxilla often involves a sinus lift, a surgical procedure to add bone to the upper jaw in the area of your molars and premolars. While effective, sinus lifts can be invasive, extend treatment time, and increase costs. Pterygoid implants are strategically placed to bypass the maxillary sinus entirely, anchoring into the dense bone of the pterygoid process. This eliminates the need for a sinus lift, reducing surgical morbidity and patient discomfort. You can learn more about traditional Sinus Lift services on our site.
Similarly, pterygoid implants often negate the need for extensive bone grafting. The inherent density of the pterygoid bone provides a stable foundation, even in cases of severe maxillary atrophy. This is a game-changer, as it avoids the healing period associated with bone grafts, leading to a significantly shortened treatment time. For patients eager to restore their smile, this means fewer appointments and a quicker return to full function.
Furthermore, the robust primary stability often achieved with pterygoid implants can allow for immediate loading, meaning a temporary prosthesis can be placed soon after surgery. This is a huge psychological and functional advantage, as patients don’t have to endure a period without teeth while waiting for healing.
From a prosthetic standpoint, pterygoid implants are invaluable for providing posterior support for prosthetics. In full-arch rehabilitations, placing implants further back in the jaw helps distribute chewing forces more evenly, significantly reducing detrimental distal cantilevers. This improved biomechanics contributes to the longevity and stability of the final restoration. The American College of Prosthodontists (ACP) supports the use of these implants, stating that they are a “scientifically validated and predictable treatment option.” You can read their official Position Statement: Use of Implants in the Pterygoid Region for Prosthodontic Treatment for more details.
Clinical Outcomes and Success Rates
The reported success and survival rates for pterygoid implants in the scientific literature are encouraging, positioning them as a reliable option for posterior maxillary rehabilitation.
- A systematic review conducted in 2011 indicated a 92% short-term survival rate for implants placed in the pterygoid region.
- A study in 2005 reported an impressive 98.6% survival rate for pterygoid implants.
- More recent research, specifically focusing on implants with modern micro-roughened surfaces, has shown an even higher 3-year survival rate of 99%.
These figures are comparable to, and in some cases, even exceed, those for other posterior maxillary implant options. This strong track record demonstrates the predictability and efficacy of pterygoid implants when performed by experienced clinicians. Long-term outcomes continue to be studied, but the existing data supports their role in successful prosthesis survival and patient satisfaction.
Risks, Complications, and Patient Selection
While pterygoid implants offer remarkable advantages, it’s crucial to acknowledge the associated risks and challenges. As with any advanced surgical procedure, understanding these elements is key to informed decision-making and optimal patient care.
One significant aspect is the learning curve and technique sensitivity. Placing pterygoid implants is not a routine procedure for every dentist. It requires a deep understanding of pterygoid implants anatomy, advanced surgical skills, and extensive experience. The precise angulation and trajectory are critical, making it a technique-sensitive procedure that demands meticulous planning and execution.
The proximity to vital structures is another major concern. As we discussed with the Greater Palatine Canal, there’s a risk of injury to the descending palatine artery and greater palatine nerve. Additionally, the internal maxillary artery and pterygoid venous plexus are in the vicinity, posing a potential for significant bleeding if inadvertently damaged. While serious complications like sectioning the maxillary artery are rare, they highlight the need for extreme caution and anatomical expertise.
Patients may also face access challenges for hygiene due to the posterior location of these implants. Maintaining proper oral hygiene around such distal implants can be more difficult, necessitating thorough patient education and consistent follow-up care. Furthermore, radiographic assessment of marginal bone loss around pterygoid implants can be challenging due to their angulation and surrounding complex bony structures, making long-term monitoring somewhat more intricate.
Indications and Contraindications for Pterygoid Implants
To ensure the best possible outcomes, patient selection for pterygoid implants is critical. We carefully evaluate each patient’s unique anatomical situation and overall health before recommending this treatment.
| Indications for Pterygoid Implants | Contraindications for Pterygoid Implants |
|---|---|
| Severe Maxillary Atrophy: When there is insufficient bone height or width in the posterior maxilla for conventional implants. | Trismus or Reduced Mouth Opening: Limits surgical access and visibility, making the procedure unduly challenging. |
| Partial Edentulism: To restore missing posterior teeth without resorting to extensive grafting procedures. | Absent Maxillary Tuberosity: If the entry point for the implant is missing, this technique cannot be performed. |
| Complete Edentulism: To provide stable posterior anchorage for full-arch fixed prostheses, especially when four implants are insufficient. | Impacted Third Molars: Can obstruct the surgical access pathway and interfere with implant placement. |
| Maxillectomy Defects: For complex reconstructions following tumor resections or trauma. | Uncontrolled Systemic Diseases: Conditions that impair healing or increase surgical risk, such as uncontrolled diabetes or severe bleeding disorders. |
| Patients Wishing to Avoid Sinus Lifts/Bone Grafts: Offers a less invasive alternative for those seeking to reduce treatment time and morbidity. | Active Infection in the Surgical Area: Must be resolved before any implant placement. |
| Need for Posterior Extensions: Enables the fabrication of prostheses with adequate posterior support, minimizing cantilevers. | Severe Pterygomaxillary Fissure Anomalies: Anatomical variations that make safe implant placement impossible. |
By adhering to these strict guidelines, we ensure that pterygoid implants are placed in suitable candidates, optimizing their chances of success and minimizing potential complications.
Pterygoid vs. Zygomatic Implants: A Comparative Overview
When faced with severe maxillary atrophy, both pterygoid and zygomatic implants emerge as viable advanced solutions, each with its own set of characteristics. Understanding their differences is key to selecting the most appropriate treatment for our patients in New York City.
Surgical complexity is a notable distinction. While pterygoid implants require a high level of surgical skill and a thorough understanding of pterygoid implants anatomy, they are generally considered less surgically complex than zygomatic implants. Zygomatic implants, which anchor into the cheekbone (zygoma), often involve a more extensive surgical field and a greater learning curve due to their proximity to vital orbital structures.
The indications for severe atrophy also differ. Pterygoid implants are excellent for moderate to severe posterior maxillary atrophy, especially when the maxillary tuberosity and pterygoid process still offer sufficient bone. Zygomatic implants, on the other hand, are typically reserved for the most extreme cases of maxillary bone loss, where there is virtually no native bone left in the posterior maxilla, or after maxillectomy procedures.
Complication rates and types vary between the two. Pterygoid implants carry risks related to the pterygomaxillary fossa, including potential injury to the descending palatine artery or nerve, or perforation into the infratemporal fossa. Zygomatic implants, while highly successful, can have complications such as sinusitis, paresthesia, or, in rare cases, orbital penetration.
In terms of prosthetic outcomes, both can provide excellent support for full-arch fixed prostheses, allowing for immediate loading and reduced cantilevers. However, the angulation of zygomatic implants can sometimes lead to more complex prosthetic designs to manage emergence profiles.
Patient comfort during and after the procedure can also differ. Pterygoid implant placement is often performed under local anesthesia, whereas zygomatic implant surgery may sometimes require general anesthesia due to its more invasive nature.
At Tribeca Dental Studio, we offer both pterygoid and zygomatic implant solutions. Our team, led by Dr. Nina Izhaky, is highly experienced in assessing your specific needs to determine which advanced implant option is best suited for your unique case. For more detailed information on options for severe bone loss, visit our page on Zygomatic Dental Implants.
Frequently Asked Questions about Pterygoid Implants
We understand that considering advanced dental implant options can bring many questions. Here are some of the most common inquiries we receive about pterygoid implants:
Why are pterygoid implants a good alternative to sinus lifts?
Pterygoid implants are an excellent alternative to sinus lifts primarily because they use existing dense bone in the pterygoid region, completely bypassing the need for invasive sinus augmentation procedures. In cases of significant bone loss in the posterior maxilla, traditional implants would require a sinus lift to create enough bone height. This procedure involves grafting bone into the sinus cavity and requires a lengthy healing period (often 6-9 months) before implants can be placed.
With pterygoid implants, we anchor directly into the robust cortical bone of the pterygoid process, which is naturally resistant to resorption. This significantly reduces surgical morbidity, eliminates the need for bone grafting, and dramatically shortens the overall treatment time and cost. For patients in Tribeca and Manhattan, this means a faster, less invasive path to a stable, functional smile.
How successful are pterygoid implants?
Pterygoid implants boast impressive success rates, making them a predictable and reliable treatment option. Scientific literature reports high success, with modern studies demonstrating excellent outcomes. A systematic review from 2011 indicated a 92% short-term survival rate, while other studies reported a 98.6% survival rate in 2005. More recent research, particularly with implants featuring micro-roughened surfaces, shows an even higher 3-year survival rate of up to 99%.
These figures are comparable to, and often exceed, the success rates of other complex implant solutions for the atrophic maxilla. This high predictability underscores why the American College of Prosthodontists considers implants in the pterygoid region a scientifically validated and predictable treatment.
What is the most critical aspect of pterygoid implants anatomy for a surgeon to know?
For a surgeon, the most critical aspect of pterygoid implants anatomy is a comprehensive, three-dimensional understanding of the implant’s trajectory through the maxillary tuberosity, the pyramidal process of the palatine bone, and its ultimate anchorage in the pterygoid process of the sphenoid bone. This includes intimate knowledge of the precise angulation required to engage the dense cortical bone effectively.
Equally vital is an in-depth understanding of the location and contents of the Greater Palatine Canal (GPC). Knowing that the GPC often has bone dehiscence and contains the descending palatine artery and greater palatine nerve is crucial. This anatomical insight allows the surgeon to maintain adequate safety margins (at least 2 mm) and avoid neurovascular complications, such as bleeding or nerve damage. Meticulous pre-surgical planning using CBCT imaging is indispensable for navigating this complex region safely and effectively.
Conclusion: A Stable Foundation for Your Smile
Pterygoid implants represent a significant advancement in dental implantology, offering a scientifically validated and predictable solution for patients with severe bone loss in the posterior maxilla. By leveraging the unique pterygoid implants anatomy, particularly the dense cortical bone of the pterygoid process, we can bypass complex and time-consuming procedures like sinus lifts and bone grafts. This innovative approach translates to shorter treatment times, reduced surgical morbidity, and often, the possibility of immediate loading, allowing our patients in Tribeca and Manhattan to enjoy a restored smile sooner.
The success of pterygoid implants, with reported survival rates up to 99%, hinges on a deep understanding of the intricate anatomy of the pterygomaxillary region. This includes precise knowledge of key bony structures, bone density variations, and the critical location of neurovascular bundles within the Greater Palatine Canal. This is why the expertise of your implant surgeon is paramount.
At Tribeca Dental Studio, Dr. Nina Izhaky and our dedicated team combine state-of-the-art diagnostic tools, meticulous planning, and extensive surgical experience to ensure the highest standards of care. We believe that everyone deserves a stable foundation for their smile, and with a thorough understanding of pterygoid implants anatomy, we can provide predictable and life-changing results.
Ready to explore how advanced implant solutions can transform your smile? Restore your smile with advanced implant solutions at Tribeca Dental Studio.

